Wisdom teeth surgery typically takes 45 minutes to 1 hour, depending on how many teeth are being removed and their complexity. A simple extraction of one erupted tooth may take as little as 20 minutes, while removing four impacted wisdom teeth could stretch the procedure to over an hour.
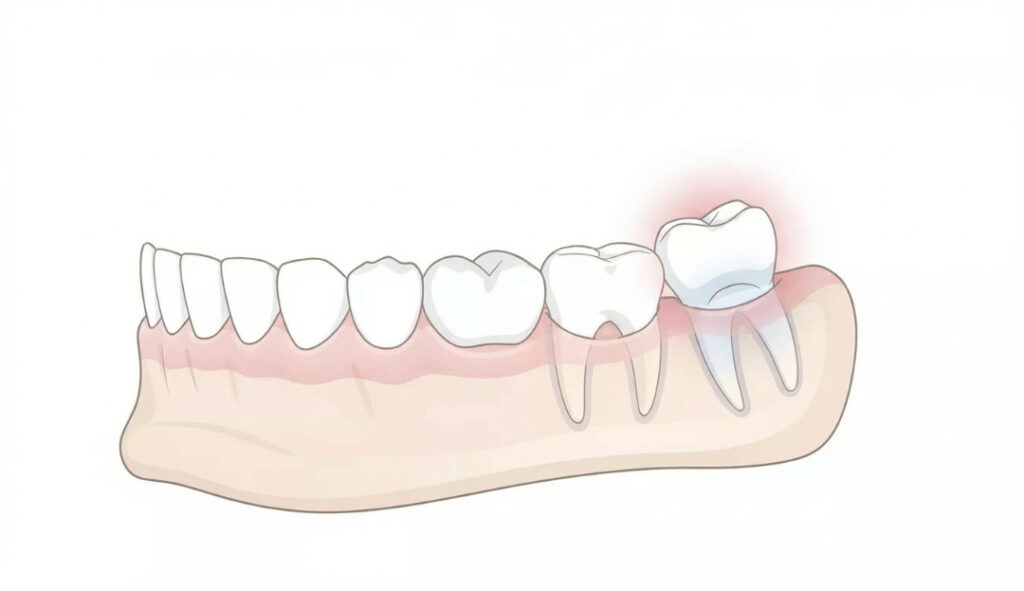
Wisdom teeth, also known as third molars, usually emerge between ages 17 and 25. In many cases, they cause problems due to lack of space in the jaw, leading to:
Not everyone needs wisdom teeth removed, but if they are impacted, growing at an angle, or causing oral health issues, extraction becomes essential. At Buford Dentist, we evaluate your unique condition to determine whether surgery is necessary.
The average surgery time for wisdom teeth removal is between 45 minutes to 1 hour. The timeline varies depending on several factors:
Same-day surgery is standard practice. You'll arrive, undergo the procedure, recover from anesthesia, and return home within a few hours.
Several variables can influence how long your wisdom teeth extraction will take:
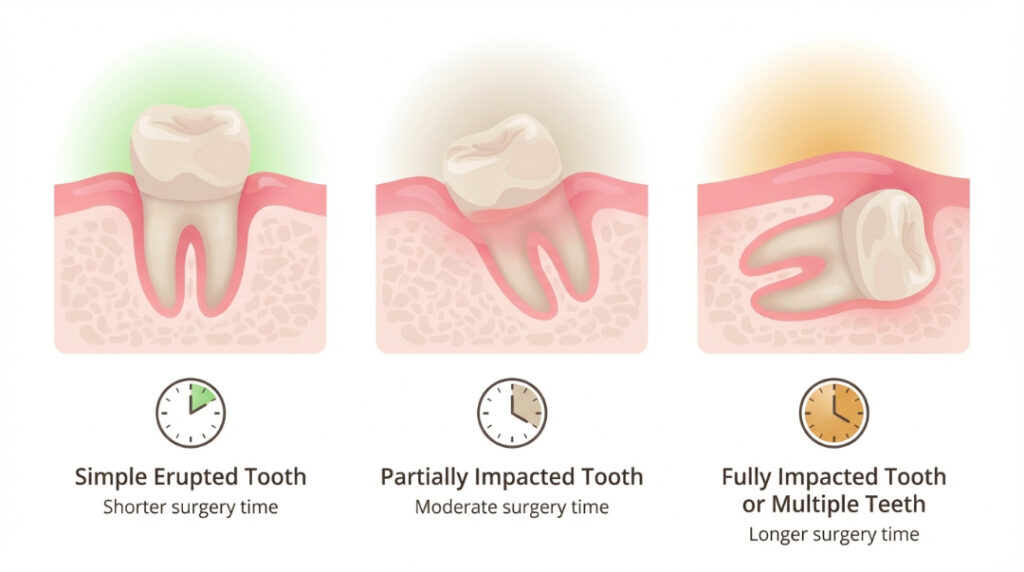
Time: 15 to 25 minutes
Time: 60 to 90 minutes
![What Happens During the Procedure? [Step-by-Step Guide]](https://buforddentist.com/wp-content/uploads/2025/12/buforddentist-what-happens-during-the-procedure-step-by-step-guide-1024x585.jpg)
In extremely rare cases, a no anesthesia extraction is performed—typically only when anesthesia isn’t an option due to medical concerns or patient refusal. These cases are highly painful and not generally advised.

After the procedure, most patients stay at the clinic for 30–60 minutes for monitoring. Here's what to expect in the first few hours:

Recovery time varies, but here’s a general guideline:
Eating the right foods can speed up recovery and reduce discomfort. For a complete list of what to eat (and what to skip), check out our Post-Surgery Eating Guide.
With proper anesthesia, the procedure is painless. Post-op soreness is common but manageable with medication.
Many patients return within 2 to 3 days, depending on the surgery's complexity.
Persistent bleeding beyond 24 hours,
Severe swelling or fever,
Foul taste or pus (signs of infection),
Dry socket (intense pain 2–3 days post-op)
Contact Buford Dentist if you notice signs of infection, prolonged bleeding, or unmanageable pain.
If you're planning to have all four wisdom teeth removed, expect:
At Buford Dentist, we help make the entire process safe, efficient, and as comfortable as possible. Whether you're facing a simple extraction or a complex case, our expert team is here to guide you from start to finish.
Yes, you can eat—but only soft, cool, and gentle foods for the first few days after wisdom teeth removal. Avoid anything hard, crunchy, spicy, or sticky to prevent complications like dry socket and delayed healing.
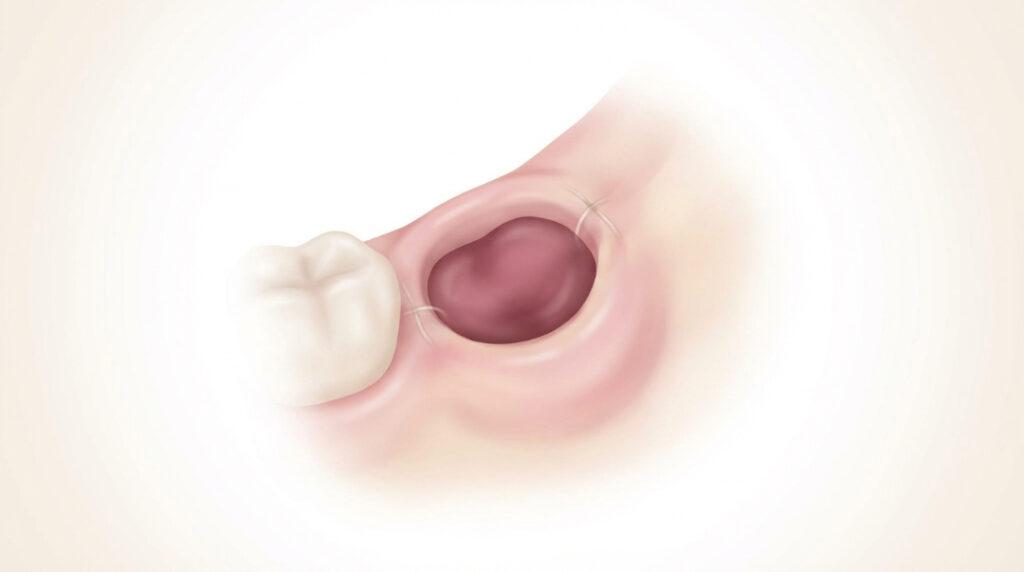
After your wisdom teeth are removed, your mouth goes through several healing stages. Each phase affects what you can—and can't—safely eat.

Your food choices impact how fast—and how well—you heal. Eating the wrong things can lead to infection, pain, or longer downtime.


Why: These can irritate the surgical site or dislodge blood clots.
Why: Chewing puts pressure on healing areas and increases risk of injury.
Why: Heat and spice can increase inflammation and irritate healing tissue.

Stick to soft, nourishing meals during the first two weeks and avoid foods that can harm your healing gums—smart eating is a key step toward faster wisdom teeth recovery.
No, avoid pizza for at least 1–2 weeks. The crust is too chewy and may dislodge clots or strain healing tissues.
Yes, ramen is okay after the first 48 hours, as long as it’s lukewarm and not spicy. Use a spoon instead of slurping to avoid pressure changes in your mouth.
Yes, soft white bread (without crust) is fine after 4–5 days. Avoid toasted or crusty types which may irritate the surgical site.
Yes, well-cooked and soft pasta is safe around days 2–3. Avoid hot sauces and stick to smooth textures.
Yes, soft noodles are safe if they’re not hot or spicy. Chew gently and eat slowly to avoid disturbing the clot.
Yes, mac and cheese is perfect after day 3. Its soft texture makes it easy to eat while still being filling.
Yes, soft rice is okay around day 4. Mix it with broth or sauce to prevent grains from sticking in the extraction site.
No, toast is too crunchy and can injure healing gum tissue. Wait at least two weeks before eating anything with a crispy texture.
Yes, shredded or boiled chicken is safe after 4–5 days. Avoid fried or grilled versions that are too chewy.
Soft meats like ground beef are okay after 5–7 days. Avoid tougher cuts like steak until week 2 or later.
Yes, eggs are one of the best recovery foods. Scrambled or soft-boiled eggs are easy to chew and nutrient-rich.
No, steak is too tough and requires too much chewing. Wait at least 2 weeks before attempting steak.
No, bacon is both chewy and crunchy—two textures to avoid. It can irritate or tear the healing site.
Yes, soft ground beef is easy to chew and can be eaten after 5 days. Use it in soups or with soft pasta.
After a week, yes, if they’re not overly crunchy. Soften them with sauce and chew gently.
Yes, after 7–10 days if the bun is soft and the patty isn’t tough. Chew slowly and avoid biting directly onto the healing area.
No, tacos are too crunchy and contain sharp ingredients. Wait until you’re fully healed before eating them.
Yes, soft cheeses like mozzarella or cream cheese are safe after day 2. Avoid firm or aged cheeses early on.
Yes, smooth yogurt is perfect from day 1. Avoid varieties with chunks, seeds, or granola.
Yes, ice cream soothes swelling and is great on day 1. Avoid flavors with nuts or mix-ins that require chewing.
Yes, cottage cheese is high in protein and very soft. It’s a great option starting on day 2.
No, fries are too hard and crunchy for the first week. Even soft fries can break into sharp pieces that irritate wounds.
No, chips are one of the worst offenders for dry socket. Skip them completely for at least 2–3 weeks.
Soft cookies may be okay after 7 days. Avoid hard or crunchy ones until fully healed.
Yes, moist cakes are okay after about a week. Avoid dense cakes with nuts or chunks.
Yes, soft chocolate that melts in your mouth is fine after 5–7 days. Skip anything with nuts or sticky centers.
Avoid candy for 1–2 weeks. Sticky and hard candies pose a high risk to healing tissue.
Yes, soft donuts are generally safe after 5–7 days. Be cautious with filled or glazed types that may stick to your gums.
Fruits & Vegetables
Yes, bananas are soft and ideal from day 1. Mash them if needed to make swallowing easier.
Yes, applesauce is smooth, soothing, and easy to eat. It’s a top choice for day 1 recovery.
Yes, mashed potatoes are one of the best healing foods. Make them smooth and lukewarm.
Only soft or cooked vegetables are safe in the first week. Avoid raw or crunchy ones until you’re fully healed.
Wait 5–7 days to eat salad. Raw greens can get trapped in the socket and disrupt healing.
Texture, Temperature & Spice
No, crunchy food can tear healing tissue or dislodge clots. Avoid for 2–3 weeks or until cleared by your dentist.
No, hard food should be avoided entirely during early healing. It increases your risk of bleeding or dry socket.
No, spicy food can irritate open wounds and cause inflammation. Wait until your mouth has fully healed.
Avoid very hot food for the first 3–4 days. Stick to lukewarm meals to protect healing tissues.
No, sticky foods can pull at stitches or the clot, leading to complications. Avoid them for at least 1–2 weeks.
After wisdom teeth removal, avoid hot, carbonated, and alcoholic beverages for at least 24–72 hours. Stick with room-temperature water, lukewarm herbal teas, and nutrient-rich drinks without using a straw. Drinking the wrong thing can cause serious complications like dry socket.

Your drink choices immediately after oral surgery can directly affect how quickly and safely you heal. Choosing the wrong beverage may delay your recovery or even cause painful complications.

Only consume soft, non-acidic, and cool or lukewarm beverages. Avoid anything that could burn, irritate, or disturb the extraction site.
Best options:
Once bleeding has fully stopped and you’re less swollen, you can introduce more nutritious drinks.
You can safely consume:
As healing progresses, your options increase. However, caution is still needed with heat and acidity.
Drinks you can enjoy (especially if you're wondering can you drink coffee after extraction):

Choosing drinks that promote healing is smart. Go for ones packed with hydration, protein, and anti-inflammatory nutrients.
Top healing drinks:
These support:

For the first 72 hours, steer clear of:
Drinking soda after wisdom teeth removal is especially risky—carbonation and acidity can disrupt healing and increase the chance of dry socket. Learn more about Soda After Wisdom Teeth Removal.
Why avoid them?
| Timeframe | Safe Drinks | Avoid |
| 0-24 Hours | Water, broths, lukewarm herbal teas | Hot drinks, soda, alcohol, acidic juices |
| 2-5 Days | Smoothies, milk, protein shakes | Citrus juice, carbonated drinks, straws |
| 2-5 Days | Cold brew, coconut water, diluted apple juice | Strong alcohol, high-caffeine drinks |
Short answer: Don’t.
Using a straw—even gently—can suck the clot right out of your socket. This can lead to dry socket, which is not only painful but also delays healing for several days.
Rule of thumb:

Fueling your body from the inside helps wounds close faster and keeps your energy up during recovery.
Tip from Buford Dentist:
Stick to room temperature and blend until smooth—avoid seeds, skins, or thick textures early on.
FAQ: What Can You (and Can’t) Drink After Wisdom Teeth Removal?
Coffee & Tea
Yes, after 24 hours. Stick with lukewarm temperatures to avoid damaging the healing tissue or dissolving the blood clot. Hot coffee too soon can trigger dry socket.
Yes, after the first 24 hours. Just avoid using a straw, as the suction can dislodge the clot and slow healing. Sip slowly from a cup instead.
No, avoid it for at least 24 hours. Heat can disrupt clot formation, increasing your risk of infection and dry socket.
Yes, as long as it’s lukewarm and consumed after 24 hours. Even without caffeine, the temperature matters more during early healing.
Avoid hot tea in the first 24 hours. You can introduce lukewarm herbal teas after that to help reduce inflammation and promote relaxation.
Yes, lukewarm herbal teas like chamomile or peppermint are safe. These can soothe the surgical site and even aid in reducing swelling.
Yes, once 24 hours have passed. Just be sure to avoid straws and excessive cold which might irritate sensitive gums.
Avoid it for at least 24–48 hours. It’s both hot and often sugary, which can irritate the extraction site and raise risk of infection.
Juices & Smoothies
Yes, but stick with non-acidic options like diluted apple juice. Avoid anything citrus-based early on due to its irritating acidity.
No, orange juice is too acidic and can sting the surgical area. Wait at least 3–5 days before reintroducing it.
Yes, after the first 24 hours. It’s mild and non-acidic, but still best when diluted and consumed at room temperature.
Yes, smoothies are great after 24–48 hours. Make sure they’re seedless and smooth in texture, and never use a straw.
Yes, and they’re a great source of healing nutrients. Just remember to drink directly from a cup to avoid creating suction.
Milk & Dairy
Yes, lukewarm milk is safe and can provide calcium and protein. Skip the straw and avoid very cold temperatures.
Yes, but in moderation. Make sure it’s not too cold and that you’re sipping it slowly from a cup.
Yes, as long as it’s not too cold and you're not using a straw. Cold temperatures may cause sensitivity in healing tissues.
Yes, Ensure and similar meal replacement drinks are nutrient-dense and easy to swallow. Always consume them without a straw.
Water & Hydration
Yes, and it can even help reduce swelling in the first 24 hours. Just sip slowly and avoid swishing or spitting.
Yes, but be cautious with very cold items as they may trigger pain or sensitivity. Stick to lukewarm or cool over icy.
Yes, but choose low-sugar versions or dilute them with water. Gatorade helps replenish lost electrolytes, especially if you’ve been groggy or haven’t eaten much.
Yes, Pedialyte is a great option for rehydration. It’s gentle and full of electrolytes, making it ideal post-surgery.
Soda & Carbonated Drinks
No, avoid for at least 48–72 hours. The carbonation can dislodge your blood clot and sugar can promote bacterial growth.
No, Coke is both carbonated and acidic, which makes it doubly risky. Wait several days before reintroducing.
No, despite being lighter, Sprite is still carbonated and can affect your healing site. Avoid for at least two days.
Avoid it for the first 2–3 days. Even unflavored sparkling water can cause bubbling at the extraction site, risking clot disruption.
No, carbonation increases the chance of dry socket and slows recovery. Wait until your oral surgeon clears you.
Alcohol
No, wait at least 72 hours. Alcohol thins your blood and may interact negatively with painkillers or antibiotics.
Avoid alcohol entirely for 72 hours or longer. It interferes with healing, increases bleeding risk, and may numb you to signs of infection.
No, wine is acidic and alcoholic, both of which hinder healing. Wait several days and consult your dentist.
No, hard liquor is especially harsh on healing tissues. Delay consumption until the site is fully closed and you're off medications.
Miscellaneous
No. The suction can dislodge the healing clot and cause a dry socket. Avoid all straws for at least 7 days.
Avoid for at least 72 hours. Energy drinks are often highly caffeinated and sugary, both of which can interfere with proper recovery.
You should wait at least two weeks before eating chips after wisdom teeth removal for upper extractions and up to eight weeks for lower extractions, as they heal slower. Crunchy foods can dislodge the blood clot, leading to painful complications like dry socket. Always consult your Buford Dentist before reintroducing chips into your diet.
Wisdom teeth removal is a common dental procedure, but the recovery process requires careful attention—especially regarding what you eat. One of the most frequently asked questions is: When can you eat chips after wisdom teeth removal? The short answer: At least two to eight weeks, depending on your extraction site and healing progress.
Eating crunchy foods too soon can disrupt healing, increase the risk of dry socket, and cause unnecessary discomfort. However, once your gums have sufficiently healed, you can carefully reintroduce crunchy snacks like chips with some precautions.
Dry socket occurs when the protective blood clot covering the extraction site becomes dislodged or dissolves too early. Chips, due to their hard, jagged texture, can easily disturb the clot, leading to exposed bone and intense pain.
Even if you think you're healing well, chips can be sharp and may scratch or irritate the extraction site. This can cause inflammation and prolong the healing process.
Small food particles, especially from crunchy snacks, can get lodged in the healing area, leading to infection or irritation. Unlike soft foods, chips are difficult to rinse away completely, making them a potential hazard during early recovery.

Once you've waited an appropriate amount of time, follow these precautions:

If you’re craving something crunchy, here are some safer options while you wait:
Before you reach for a bag of chips, ensure you meet these criteria:
If you experience any of the following after eating chips, contact your Buford Dentist immediately:
Your dentist can provide personalized guidance on your healing progress and whether it's safe to reintroduce crunchy foods into your diet.
While you may be eager to snack on your favorite chips after wisdom teeth removal, waiting at least 2 to 8 weeks ensures a safe, complication-free recovery. Prioritize soft foods, listen to your dentist’s recommendations, and gradually reintroduce crunchy snacks once your gums have healed. When in doubt, schedule a consult at Buford Dentist for expert advice on your post-surgery diet.
Gums can recede to the point where teeth become loose and eventually fall out, typically when the recession reaches 5mm or more and significant bone loss occurs. Early intervention is crucial to prevent further deterioration. If you notice signs of gum recession, consult a dentist immediately to avoid severe consequences.
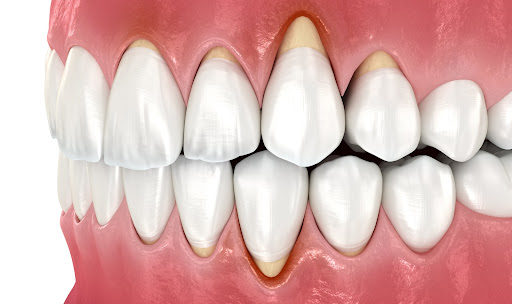
Gum recession occurs when the gum tissue surrounding the teeth pulls back, exposing more of the tooth or its root. This process can be gradual, making it difficult to notice until severe symptoms develop. Unlike general gum disease, which affects the entire gum structure, gum recession specifically involves the loss of gum tissue, often leading to sensitivity, aesthetic concerns, and, in extreme cases, tooth loss.
Several factors contribute to gum recession, including:
Gum recession progresses through several stages, each increasing the risk of tooth instability and loss.
Tooth longevity with gum disease largely depends on how far the gums have receded and the extent of accompanying bone loss. Teeth typically become loose and fall out when gum recession reaches 5mm or more, combined with periodontal deterioration.
As gums recede, the underlying alveolar bone may also deteriorate. This bone supports the teeth, and when it breaks down due to gum disease, the teeth lose their foundation and become loose. Advanced periodontal disease is often irreversible and requires immediate dental intervention.
While gum tissue does not grow back naturally, certain steps can slow or halt the progression of gum recession.
If gum recession is already severe, several treatments can help restore gum health and prevent tooth loss.
Once gum tissue is lost, it does not regenerate naturally. However, certain treatments like gum grafting can restore lost tissue. Future advancements, such as stem cell research and regenerative medicine, may provide new solutions for gum tissue restoration in the coming years.
New advancements in dental care continue to improve gum recession treatment. Some promising innovations include:
Gum recession is a progressive condition that, if left untreated, can lead to tooth loss. When recession reaches 5mm or more, teeth become unstable due to bone deterioration. Early intervention is key—whether through proper oral care, lifestyle changes, or professional treatment.
Yes, you can get your wisdom teeth removed while pregnant in certain situations, but the timing matters. The second trimester is considered the safest period if removal is necessary, while the first and third trimesters pose higher risks. Always consult both your dentist and OB-GYN to create a safe treatment plan that balances your oral health and your baby’s well-being.
Wisdom teeth are the last molars that erupt, usually between ages 17 and 25. Many people experience crowding, pain, or impaction when they come in.
During pregnancy, hormonal changes increase blood flow to the gums and raise the risk of swelling, gingivitis, and infection. This can make existing wisdom tooth issues worse. Pain, inflammation, or infection in the gums can become harder to manage during this time.

The answer depends on the trimester. Each stage of pregnancy brings different risks and considerations.
The first trimester is critical for the baby’s development. Major organs are forming. Medical experts typically recommend avoiding dental surgery at this stage unless the issue is life-threatening. Even though local anesthesia is generally safe, exposure to stress and medications is best minimized early in pregnancy.
The second trimester is considered the safest time for dental procedures. The baby’s major development is complete, and the risk of complications is lower. Most dentists and OB-GYNs agree that if surgery is unavoidable, this is the ideal window.
By the third trimester, lying back for a long procedure can put pressure on blood vessels and reduce circulation. This increases the risk of discomfort, fainting, or even preterm labor. Unless an emergency arises, dentists often recommend postponing surgery until after birth.
Local anesthesia, such as lidocaine, is generally considered safe during pregnancy. Dentists avoid high doses and always use the lowest amount required.
General anesthesia and nitrous oxide are not recommended during pregnancy due to potential risks to the baby. Most procedures are done under local anesthesia only.
Modern dental X-rays use very low radiation. With protective lead aprons, exposure is minimal. X-rays are only taken if absolutely necessary, such as to identify infection or impacted teeth.
Untreated oral infections pose significant dangers. Gum or tooth infections can spread into the bloodstream, increasing risks for both the mother and baby. Severe infections have been linked to preterm birth and low birth weight.
If removal is not urgent, dentists often recommend temporary treatments until after delivery.
There are situations when delaying surgery is not an option.
Signs that immediate extraction is needed:
In these cases, the risk of not treating the condition outweighs the risks of surgery. Your dentist and OB-GYN will coordinate care to ensure safety, and may recommend a timely tooth extraction to stop the infection and protect both you and your baby.

If your situation is not an emergency, most dentists recommend postponing extraction until after delivery.

The American Dental Association and the American College of Obstetricians and Gynecologists both provide clear guidance:
General anesthesia is not recommended during pregnancy due to risks to the fetus. Local anesthesia is the standard choice.
The second trimester is the safest period for dental surgery.
Acetaminophen is safe. Ibuprofen and aspirin should be avoided.
Most patients do well by delaying unless infection spreads. Pain can be managed with temporary measures until postpartum.

If you live in Georgia, it is important to coordinate care between your OB-GYN and your dentist.
Cities like Atlanta, Savannah, Augusta, and Athens have specialists experienced in treating pregnant patients with dental emergencies. Buford Dentist provides consultations and safe treatment planning for expectant mothers.


Pregnancy does not mean all dental care must stop. Preventive care is encouraged to avoid complications later.
Maintaining oral health is a key part of prenatal care. Gum disease and untreated infections have been linked to preterm labor. Regular dental visits help monitor risks and prevent complications.
Wisdom teeth removal during pregnancy is sometimes necessary, but timing and planning are critical. The safest approach is to treat emergencies promptly while delaying elective procedures until the second trimester or after delivery. By working closely with your OB-GYN and dentist, including trusted practices like Buford Dentist, you protect both your oral health and your baby’s safety.
No, you should not drink soda after wisdom teeth removal. The carbonation can disrupt healing, the acidity can irritate the extraction site, and the sugar increases the risk of infection. It’s best to wait at least one to two weeks before reintroducing soda and choose safer alternatives in the meantime.
After having your wisdom teeth removed, proper aftercare is essential for a smooth recovery. Many patients wonder if they can resume their usual diet, particularly when it comes to drinking soda. The short answer is no—drinking soda after wisdom teeth extraction can lead to complications like dry socket, irritation, and delayed healing.
To understand why soda should be avoided, let’s break down how it affects your mouth post-extraction, the risks involved, and when it’s safe to drink soda again.
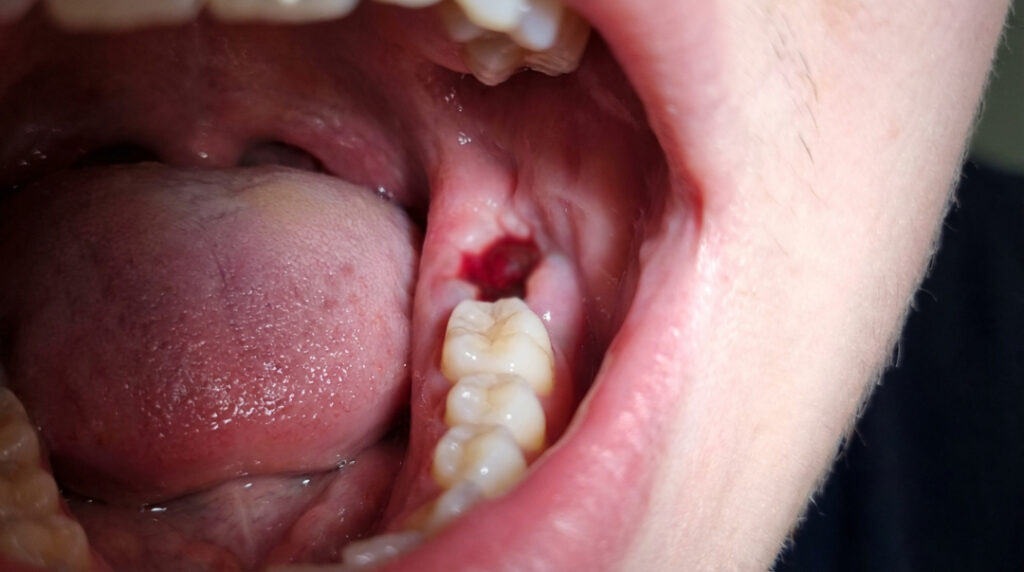
Wisdom teeth removal is a surgical procedure that requires a careful healing process. After the extraction, a blood clot forms over the wound, protecting it and allowing new tissue to regenerate. This clot is crucial—if it becomes dislodged or dissolves too soon, it can lead to painful complications like dry socket.
Healing happens in several stages:
In some cases, wisdom teeth extraction can also impact the temporomandibular joint (TMJ), leading to jaw stiffness or discomfort. If you're experiencing jaw pain or clicking after removal, check out Wisdom Teeth & TMJ to learn how they are connected and what you can do about it.
Certain factors can slow or complicate recovery, including:
This is why avoiding certain foods and drinks, including soda, is crucial in the early recovery period.

While soda may seem harmless, it poses multiple risks after wisdom teeth removal.
Soda’s bubbles come from carbonation, which can create pressure in the mouth. This pressure can dislodge the forming blood clot, leading to dry socket, one of the most painful complications of tooth extraction.
Additionally, carbonation may cause irritation and discomfort around the healing site, prolonging the recovery period.
Soda is both acidic and high in sugar, which is a bad mix for a healing mouth.
Drinking soda—especially through a straw—creates suction pressure in the mouth. This can pull the blood clot from the extraction site, leading to dry socket, which exposes the bone and nerves beneath, causing intense pain and requiring additional treatment.
Always consult with your dentist, such as Buford Dentist, for personalized recommendations on when it’s safe to resume normal dietary habits.

If soda is off-limits, what can you drink instead? The best choices are hydrating, non-irritating beverages that promote healing.
Some drinks can delay healing and increase discomfort, including:

Craving soda but need a safer alternative? Try these:

Oral surgeons widely agree that soda should be avoided in the first stages of recovery. Buford Dentist advises patients to stick to gentle, non-carbonated, and sugar-free beverages for at least one to two weeks after surgery.
Many patients who drank soda too soon reported:
Those who followed their dentist’s advice and avoided soda experienced faster, smoother recoveries with fewer complications.
Can I drink Sprite after wisdom teeth removal?
No. Despite being a clear soda, Sprite is carbonated and acidic, posing the same risks as other sodas.
What is the best juice to drink after tooth extraction?
Apple or pear juice (diluted) is best. Avoid citrus juices like orange juice due to their acidity.
Is sparkling water safer than soda after wisdom teeth surgery?
No. While it lacks sugar, sparkling water is still carbonated and can disrupt healing.
When can I drink Coke after getting my wisdom teeth out?
You should wait at least one to two weeks before drinking Coke, depending on your healing progress.
Drinking soda after wisdom teeth removal is not recommended due to the risks of dry socket, irritation, and infection. The carbonation, acidity, and sugar content can slow down healing and cause unnecessary complications.
For a smooth recovery, stick to water, herbal teas, and electrolyte-rich drinks while avoiding carbonated beverages for at least one to two weeks. If you have concerns, consult Buford Dentist for expert guidance on post-surgery care.
Dental implants are a long-term solution for replacing missing teeth, offering durability, improved oral function, and a natural appearance. The Dental Implant Procedure involves multiple stages, including consultation, surgery, healing, and crown placement. While highly effective, implants require sufficient bone density, proper oral hygiene, and can be costly.

A dental implant is a permanent tooth replacement option consisting of a titanium post that acts as a tooth root, an abutment, and a crown that mimics a natural tooth. Unlike dentures or bridges, implants fuse with the jawbone (osseointegration), ensuring long-term stability and preventing bone loss.
There are two main types:

A dentist at Buford Dentist will assess your oral health, bone density, and overall suitability for implants through X-rays or CT scans. Conditions like gum disease or bone loss may require treatment before implantation.

Ideal candidates:
Not everyone is eligible for implants. If you're wondering whether you qualify, contact us to see if this treatment is right for you.
Certain conditions (e.g., diabetes, osteoporosis, smoking) may affect healing and increase implant failure risks. In such cases, Buford Dentist may recommend alternative options like bridges or dentures. However, for patients missing several teeth, Multiple Tooth Implants can provide a stable and long-lasting solution.

The cost depends on factors such as:
A single implant can range from $3,000 to $6,000, while full-mouth implants can exceed $20,000. Some dental insurance plans cover parts of the procedure, but financing options are also available at Buford Dentist.

If implants aren’t suitable, other options include:
The procedure is done under anesthesia, so pain is minimal. Some discomfort during recovery is expected but manageable with medication.
With proper care, implants can last 20 years or more, often a lifetime.
Yes, if you prioritize durability, aesthetics, and oral health. Despite the upfront cost, their longevity and benefits outweigh alternatives.
Dental implants are a life-changing solution for those with missing teeth, offering unparalleled stability, function, and aesthetics. However, they require commitment in terms of cost, time, and proper maintenance. If you're considering dental implants, Buford Dentist can guide you through the process, ensuring the best possible outcome.
Veneers last 10 to 25 years depending on the material, care, and your habits. Porcelain veneers often last 15 to 25 years, while composite veneers usually last 5 to 12 years. Good oral hygiene, avoiding damaging habits, and regular visits to Buford Dentist extend their lifespan.
Porcelain veneers generally last 15 to 25 years. Composite veneers typically last 5 to 12 years.
The difference comes from material strength, stain resistance, and bonding techniques.
In Georgia, patients who maintain good oral hygiene and avoid harmful habits often see porcelain veneers last beyond two decades.
Key averages:

Porcelain dental veneers are durable, stain resistant, and retain natural shine. They often last more than 20 years.
Composite veneers are cheaper but less durable. They stain easier and usually need replacement within 5 to 10 years.
Newer ultra-thin porcelain and improved bonding systems are extending veneer lifespans even further.
The skill of your cosmetic dentist directly impacts veneer longevity. At Buford Dentist, precise enamel preparation and high-quality bonding improve veneer stability.
Poorly fitted veneers often fail early. High-quality lab work ensures strength and a natural look.
Healthy gums and teeth are critical. Gum disease or decay underneath shortens veneer lifespan.
Tooth structure left after preparation must be strong enough to support veneers.
Neglecting gum health or ignoring cavities under veneers leads to failure.
Knowing when veneers need replacement prevents bigger problems.
Common signs veneers should be replaced:
Most patients replace porcelain veneers after 15 to 20 years. Composite veneers usually need replacement within 5 to 7 years.
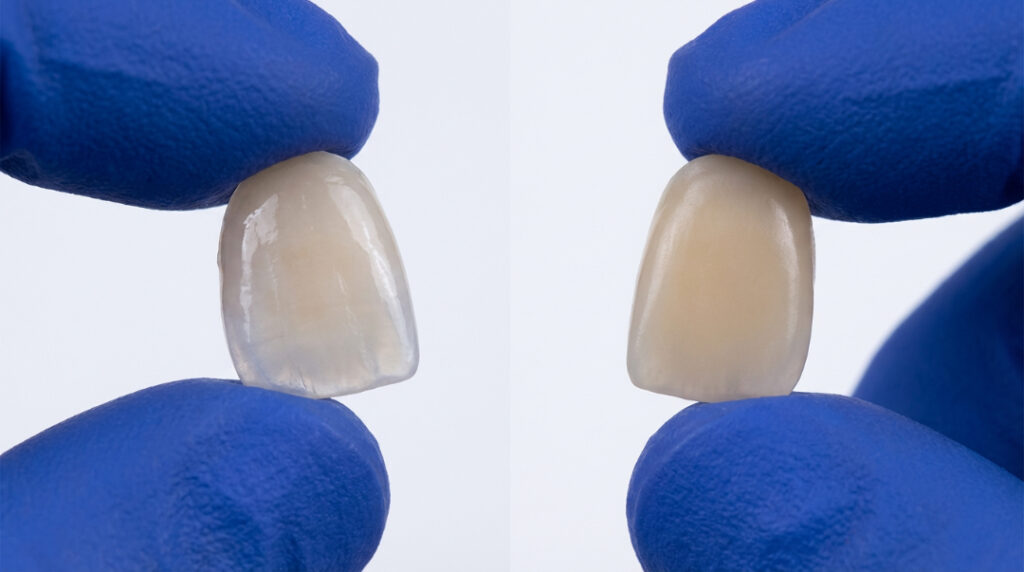
Porcelain:
Composite:
Many patients choose to fix tooth imperfections with veneers, but not everyone is a candidate. Other options exist.
Patients at Buford Dentist often weigh cost, durability, cosmetic needs, and review the pros and cons of veneers before choosing.

Porcelain veneers in Georgia range from $1,000 to $2,500 per tooth. Composite veneers range from $500 to $1,500 per tooth.
Prices depend on dentist expertise, lab work, and number of veneers.
Insurance rarely covers cosmetic veneers, but financing options are available.
Typical Georgia cost breakdown:
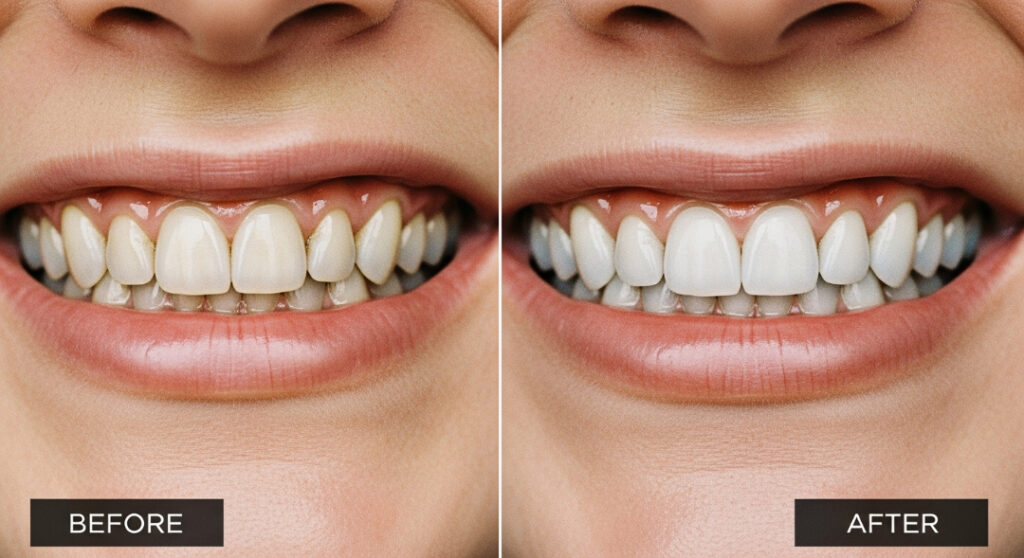
A patient in Buford received porcelain veneers in 2002. With consistent hygiene, nightguard use, and regular dental visits, their veneers lasted 22 years before replacement. The main cause of replacement was gum recession, not veneer damage.
This shows that with proper care, porcelain veneers can last well beyond average expectations.
Veneers are not permanent. They usually last 10 to 25 years depending on material and care.
If bonding weakens or tooth health declines, veneers may loosen. A dentist can re-bond or replace them.
Placing veneers involves removing some enamel. Patients usually experience mild sensitivity at first, but not pain.
Porcelain veneers resist staining. Composite veneers stain faster and need polishing or replacement sooner.
Veneers do not respond to whitening treatments. If they discolor, replacement is the solution.
Composite veneers: 5 to 10 years
Porcelain veneers: 15 to 25 years
High humidity itself does not damage veneers, but gum health and consistent dental care remain critical.

To make veneers last longer, focus on:

Porcelain veneers usually last 15 to 25 years. Composite veneers last 5 to 12 years. Your care routine and dentist skill level make the biggest difference.
At Buford Dentist, patients who commit to oral hygiene, avoid damaging habits, and attend regular checkups often enjoy long-lasting results and a confident smile with veneers in Buford.
Brushing your teeth with baking soda can be safe and effective for whitening and neutralizing acids, but it lacks fluoride and can be abrasive, potentially leading to enamel erosion over time. To minimize risks, use it sparingly and combine it with fluoride toothpaste for better oral health.
Many people swear by baking soda as a natural teeth whitener, but is it actually safe to use for brushing? The short answer: Yes, but with caution. Baking soda has mild abrasive properties that help remove surface stains and neutralize acidity in the mouth, but overuse can erode enamel and lead to increased sensitivity. Let’s break down the benefits and risks to determine the safest way to use it.

Baking soda, or sodium bicarbonate, is a mild abrasive with alkaline properties. When used for brushing, it works in three main ways:
However, unlike fluoride toothpaste, baking soda does not strengthen enamel or protect against cavities. This means it should not be used as a complete replacement for fluoride toothpaste.

Baking soda is a common ingredient in many commercial Teeth Whitening toothpastes because it effectively removes surface stains. However, it does not change the natural color of teeth or whiten deep stains like professional treatments.
A high-acid diet can weaken enamel and promote cavities. Baking soda neutralizes these acids, creating an environment less hospitable to bacteria.
Research suggests that baking soda can reduce plaque buildup by breaking down biofilm, which is a sticky layer of bacteria that contributes to cavities and gum disease.
Baking soda is significantly cheaper than commercial toothpastes and is available in most households, making it an economical option for oral care.
Frequent use of baking soda can gradually wear down enamel, leading to increased sensitivity and vulnerability to cavities.
Fluoride is essential for strengthening enamel and preventing cavities. Baking soda alone does not contain fluoride, making it less effective at protecting against decay.
Because baking soda is abrasive, people with sensitive teeth may experience discomfort or worsening sensitivity with prolonged use.
If you have crowns, veneers, or braces, baking soda’s abrasiveness can damage their surface, potentially leading to discoloration or reduced lifespan.
To minimize the risks and maximize the benefits, follow these steps. For more expert advice on proper brushing techniques, check out Toothbrushing Tips from a Dentist.
| Whitening Method | Effectiveness | Safety | Cost | Best For |
| Baking Soda | Moderate | Medium (Can erode enamel) | Very Low | Mild Stains |
| Hydrogen Peroxide | High | Low (If overused) | Low | Deep Stains |
| Activated Charcoal | Low | Low (Abrasive) | Medium | Surface Stains |
| Oil Pulling | Very Low | High (Safe) | Medium | General Oral Health |
According to the American Dental Association (ADA), while baking soda can be beneficial in removing stains and neutralizing acidity, it should not be used as a standalone toothpaste because it lacks fluoride. Many dentists recommend using fluoride toothpaste with a small amount of baking soda occasionally for added whitening benefits.
Additionally, studies have shown that while baking soda can be less abrasive than some commercial whitening toothpaste, overuse can still contribute to enamel wear over time. Consulting a dentist, such as those at Buford Dentist, can help determine if baking soda is a safe addition to your oral care routine.

Yes, and it’s actually a recommended way to reduce the abrasiveness of baking soda while benefiting from its stain-removing properties.
If used excessively or with too much pressure, baking soda can cause gum irritation and recession over time.
It is not recommended for young children, as they need fluoride protection for developing teeth, and baking soda’s abrasiveness may be too harsh.
Yes, baking soda neutralizes odors by balancing the pH in the mouth and reducing bacteria that cause bad breath.
Yes, but it should be done cautiously and only occasionally, as hydrogen peroxide can be harsh on gums and enamel.
Baking soda can be a useful supplement to your oral care routine but should not replace fluoride toothpaste. When used correctly and sparingly, it can help remove stains, freshen breath, and neutralize acidity. However, overuse can lead to enamel erosion and sensitivity. To maximize benefits while minimizing risks, use baking soda in combination with fluoride toothpaste and consult a dentist for personalized advice.