Porcelain fixed bridges are dental prostheses that are used to replace missing teeth. They comprise a series of porcelain crowns that are fused and anchored onto the adjacent natural teeth. They are a popular option for people who have lost one or more teeth because they are natural-looking, long-lasting, and functional.
However, like any dental prosthesis, they can pose certain concerns. We will discuss the dental concerns with porcelain fixed bridges and what you can do to mitigate them.
Porcelain fixed bridges are a type of dental bridge that is used to replace one or more missing teeth. Different types of dental bridges are available, but porcelain fixed bridges are a popular option because they are natural-looking, long-lasting, and functional. They consist of a false tooth, a pontic, fused to two porcelain crowns on either side of the gap. The crowns are then anchored onto the existing teeth on either side of the missing tooth, known as abutment teeth.
Porcelain fixed bridges are not the only type of dental bridge available. Traditional bridges are similar to porcelain fixed bridges but are made of metal or ceramic materials instead of porcelain. Dental implants are a more permanent solution to missing teeth but require surgery to implant a metal post into the jawbone.
Overall, porcelain fixed bridges are a popular option for people who have lost one or more teeth and want a natural-looking, functional solution. Your dentist can help you determine if a porcelain fixed bridge is right for you based on your needs and the condition of your remaining teeth.
Fixed bridges offer several benefits, including:
Although fixed dental bridges offer several benefits, they can pose certain concerns. Here are some of the common dental concerns with them:
Decay and Gum Disease
They can make it difficult to clean your teeth and gums properly. If you do not practice good oral hygiene, you may be at risk of developing tooth decay or gum disease. Food particles and bacteria can get trapped between them and your natural teeth, forming plaque and tartar.
Fracture or Breakage
They are durable but can still fracture or break if subjected to excessive force. This can happen if you bite down on hard or sticky foods or suffer a blow to the face.
Bite Problems
They can alter your bite, which can cause problems with your jaw, teeth, and gums. If your bite is not properly aligned, it can lead to jaw pain, headaches, and tooth wear.
Discoloration
They can become discolored, especially if you smoke or smoke dark-colored foods and beverages.
Poor Fit
They need to fit snugly against your natural teeth to be effective. They can cause discomfort, pain, and irritation if they do not fit properly.
To mitigate dental concerns with fixed bridges, here are some tips you can follow:
Good Oral Hygiene
Practicing good oral hygiene is crucial when you have denal bridges. You should brush your teeth twice a day, floss daily, and use an antimicrobial mouthwash to reduce the risk of developing tooth decay and gum disease. You can also use interdental brushes to clean the hard-to-reach areas between your teeth and your porcelain fixed bridge.
Regular Dental Visits
Regular dental visits are important to maintain oral health and ensure that your dental bridge functions properly. Your dentist will check your porcelain fixed bridge for any signs of damage, decay, or gum disease and recommend any necessary treatments or adjustments.
Avoiding Chewing Hard or Sticky Foods
Avoid chewing on hard or sticky foods, such as ice, hard candy, or caramel, as they can damage or dislodge your porcelain fixed bridge. Instead, opt for softer foods, such as cooked vegetables, fruit, and lean protein.
Addressing Bite Issues
If you experience any bite issues, such as discomfort or pain when biting down, or if you notice any changes in your bite, such as a clicking or popping jaw, contact your dentist immediately. They can adjust your fixed bridge to ensure that it fits properly and does not cause any further issues.
Porcelain fixed bridges are a popular option for people who have lost one or more teeth, but they can pose certain dental concerns. To mitigate these concerns, it is important to practice good oral hygiene, visit your dentist regularly, avoid chewing hard or sticky foods, and address any bite issues promptly.
Contact us at North Atlanta Center for Cosmetic & Implant Dentistry if you would like to learn more!
Cavities do not heal on their own once a hole forms in the enamel. Early-stage tooth decay, known as enamel demineralization, can be reversed with proper care such as fluoride treatment, diet changes, and improved oral hygiene. Once the enamel is broken, professional dental treatment is required to stop further damage.

To understand whether cavities can heal without fillings, you first need to know how they form. Tooth decay begins when bacteria in your mouth feed on sugars and produce acids that attack the enamel. This process is called demineralization.
Over time, small white or brown spots appear on the enamel. These spots indicate mineral loss, but at this stage, there is no hole. If untreated, the demineralized area breaks down further, forming a cavity that penetrates the enamel and spreads to the dentin beneath.
Once decay reaches the dentin, the tooth structure is permanently damaged and cannot rebuild itself. The only way to restore the tooth is through professional dental treatment such as a filling, crown, or other restorative procedure.
Key stages of decay:

You can stop or reverse early tooth decay before a cavity forms. This stage is called the reversible stage of demineralization.
Signs of reversible decay:
During this stage, remineralization can occur naturally if the right conditions exist. Fluoride, calcium, phosphate, and saliva work together to rebuild weakened enamel.
Once the enamel is broken and a hole forms, the damage is permanent. At that point, the body cannot regenerate lost enamel, and only a filling or similar restoration can repair the tooth.
Self-assessment checklist:
If you answered yes to these, healing through remineralization might still be possible.
If your tooth is still in the early stage of decay, certain steps can encourage natural remineralization and prevent further damage. Buford Dentist recommends focusing on hygiene, nutrition, and lifestyle habits that protect enamel.
The foods you eat directly impact your oral health. To promote enamel remineralization, maintain a diet that supports strong teeth.
Fluoride remains the most effective mineral for rebuilding enamel. It helps replace lost calcium and phosphate, forming a stronger, more acid-resistant surface.
Options include:
Remineralizing gels or pastes containing calcium phosphate or nano-hydroxyapatite may also aid in enamel repair when used consistently.
Saliva acts as your mouth’s natural defense system. It helps neutralize acids, wash away food particles, and deliver minerals to the enamel surface.
Tips to support saliva flow:
Your overall health affects your oral environment. Conditions such as acid reflux or frequent vomiting introduce stomach acids that erode enamel.
Steps to protect enamel:

Even with good home care, there comes a point when professional treatment is unavoidable. When decay progresses beyond the enamel, the tooth structure becomes too compromised for natural healing.
Signs you need a filling or other dental treatment:
Common dental treatments:
If you still have older silver fillings, ask your dentist about safe Mercury Filling Replacement to restore both the appearance and safety of your smile.
Comparison: Non-invasive vs. Invasive Treatment
|
Aspect |
Non-Invasive Healing |
Filling/Restoration |
|
Stage |
Early demineralization |
Advanced decay |
|
Pain level |
None |
Mild to moderate |
|
Treatment type |
Fluoride, diet, hygiene |
Filling, crown, or root canal |
|
Cost |
Lower |
Higher |
|
Long-term outcome |
Requires strict maintenance |
Restores function and appearance |
Early intervention saves time, money, and discomfort. If you are unsure about the stage of your cavity, schedule a dental exam with Buford Dentist for accurate diagnosis and advice.

Many people try home remedies they find online. While some methods help prevent decay, they do not reverse existing holes. Buford Dentist separates fact from fiction.
Myth: Oil pulling can fill cavities.
Fact: Oil pulling can improve oral hygiene but cannot rebuild lost enamel.
Myth: Stopping sugar intake heals cavities completely.
Fact: Reducing sugar helps prevent further decay but does not repair holes.
Myth: Holes in teeth can close with herbal pastes.
Fact: Once enamel is broken, no paste or supplement can regrow it.
Myth: Sensitivity means healing is happening.
Fact: Sensitivity usually indicates enamel erosion or dentin exposure.
Myth: Children’s cavities heal as baby teeth fall out.
Fact: Untreated decay can affect permanent teeth and oral health.
Skipping dental cleanings for a year allows plaque to harden into tartar, which leads to gum disease, cavities, and potential tooth loss. Missing your annual cleaning also increases your risk of enamel erosion, bad breath, and higher treatment costs in the future. Regular professional cleanings at Buford Dentist protect both your oral and overall health.

Professional dental cleanings are more than cosmetic. They are preventive care. A dental hygienist removes plaque and tartar that brushing and flossing leave behind. They also check for early signs of gum disease, tooth decay, and even oral cancer.
At Buford Dentist, cleanings include:
Brushing and flossing are important. But they cannot remove hardened tartar. Only professional dental tools can. Without regular cleanings, plaque builds up under the gums, creating a foundation for disease.
Plaque begins forming on your teeth within hours of brushing. Over time, it hardens into tartar. Tartar traps bacteria along the gumline. Once hardened, it can only be removed by a dentist or hygienist. Skipping cleanings for a year means:
This is the earliest stage of gum disease, known as gingivitis.
Gingivitis develops quietly. You may not feel pain, but symptoms appear:
Left untreated, gingivitis can progress to periodontitis. That’s when the infection moves deeper under the gumline and starts damaging the bone that supports your teeth.
When you skip dental cleanings for a year, bacteria and acids attack your enamel. Small weak spots can form. These become cavities over time. Even with good brushing habits, missed cleanings allow decay to grow unnoticed. Once cavities form, they spread quickly without professional care.

Untreated gingivitis turns into periodontitis. This stage involves bone and tissue loss. Deep pockets form between your teeth and gums. Bacteria collect in these spaces, weakening the bone structure. Without treatment, this can lead to:
Once bone is lost, it cannot regrow naturally. Treatment becomes more complex and costly. Professional cleanings at Buford Dentist help stop this progression early.
Your mouth is connected to your overall health. Bacteria from gum infections can enter the bloodstream. This increases inflammation throughout the body. Research links gum disease to several systemic conditions:
Skipping a dental cleaning for a year doesn’t only risk your teeth. It affects your total health.
Preventive visits are inexpensive compared to restorative procedures. If you skip cleanings for a year or longer, minor issues can become major treatments. Common outcomes include:
Delaying care always costs more in the long run. Early detection during regular checkups saves both money and discomfort.

While most people should visit every six months, others may need more frequent cleanings. People with diabetes, smokers, or those with a history of gum disease are at higher risk. At Buford Dentist, we personalize cleaning schedules based on each patient’s health, not a one-size-fits-all rule.
If you have skipped your dental cleaning for a year or longer, here is how to recover:
This step-by-step approach helps reverse early damage and restores oral health.
To reduce risks between appointments:
If you smoke or have medical conditions like diabetes, you should schedule cleanings more often. Preventive care keeps issues under control.

When booking your visit, tell your Buford Dentist team it has been a year or longer. This helps the dentist prepare for a thorough cleaning and evaluation.
Getting these answers helps you create a personalized prevention plan.
Your dentist will outline a plan to restore your gum health. This may include:
Consistency is key. Once you return to a healthy routine, future visits become easier.
Follow your dentist’s recommended schedule. Signs to watch for include:
Early detection keeps problems manageable and prevents relapse.
Not immediately, but plaque and tartar build up over time. Missing one year allows bacteria to thrive, leading to gum inflammation and enamel damage. The longer you wait, the harder it becomes to reverse the effects.
For most patients, six months is ideal. People with gum disease, diabetes, or smoking habits should visit every three to four months.
Yes, early-stage gingivitis is reversible with professional cleaning and proper home care. If periodontitis has started, treatment can control but not fully reverse bone loss.
Most plans cover two cleanings a year. Take advantage of these benefits to avoid paying for costly restorative treatments later.
No. Plaque turns into tartar within days. After months, the risk of gum disease and cavities rises sharply. Annual visits prevent long-term damage.
Yes, night guards help relieve TMJ symptoms by reducing teeth grinding and clenching that strain the jaw joint. They cushion the bite, protect teeth from wear, and promote muscle relaxation, but effectiveness depends on getting a custom-fitted guard from a qualified dentist like Buford Dentist.

The temporomandibular joint, or TMJ, connects your jawbone to your skull. It is one of the most complex joints in the body, responsible for chewing, speaking, and swallowing. When the joint becomes strained or inflamed, it leads to temporomandibular joint disorder, or TMD.
Common symptoms include:
TMJ problems often start from habits like clenching or grinding your teeth at night, known as bruxism. Over time, the constant pressure wears down enamel and tightens jaw muscles, creating inflammation and misalignment.

Night guards, also called occlusal splints, are dental appliances designed to protect your teeth while you sleep. Their main purpose is to reduce the harmful effects of grinding and clenching that worsen TMJ pain.
A night guard creates a thin barrier between your upper and lower teeth. This prevents direct contact and stops the friction that causes enamel erosion and joint strain. The cushioning absorbs the force of clenching, allowing the jaw muscles to relax overnight.
A well-designed guard positions your jaw in a balanced, neutral state. This reduces muscle tension and helps relieve the stiffness you might feel in the morning. Many patients notice a drop in headaches and soreness after consistent use.
When grinding decreases, your muscles relax and your sleep becomes deeper. Rested muscles are less inflamed, leading to less jaw pain, fewer morning headaches, and a calmer nervous system overall. Since sleep quality directly affects jaw tension, exploring the link between TMJ and Sleep Habits can help you understand how rest impacts long-term relief.
Night guards are a proven tool for managing TMJ symptoms. Yet, their success depends on the cause of the disorder and the quality of the appliance.
They work best when:
In these cases, the guard minimizes grinding and relieves muscle tension that contributes to TMJ discomfort.
If TMJ pain stems from arthritis, severe misalignment, or joint damage, a night guard alone will not solve the problem. Some patients require additional care such as orthodontic correction, physical therapy, or medication to reduce inflammation.
Store-bought guards, especially boil-and-bite versions, may seem convenient but often fit poorly. A poor fit can worsen your bite, strain your muscles further, or even lead to more pain.
A comprehensive TMJ treatment plan may also include:
Buford Dentist emphasizes that night guards are one part of a larger management plan, not a standalone cure.

Choosing the correct guard is essential to achieve lasting TMJ relief.
Custom night guards are designed using impressions of your teeth. They fit precisely, stay secure, and distribute pressure evenly across the bite. Over-the-counter versions are mass-produced and rarely align correctly. This mismatch can cause additional jaw strain or gum irritation.
Dentists choose between upper and lower guards based on your bite pattern and comfort.
The best choice depends on your anatomy and the source of your TMJ stress, which Buford Dentist evaluates before recommending one.
Hard acrylic guards are durable and stabilize the bite for severe clenchers. Soft guards cushion better but wear down faster and may encourage more chewing movements. Hybrid versions combine both materials to balance comfort and durability.
When selecting a night guard, check for:
Custom guards cost more upfront but last longer and protect dental work from costly repairs. Over-the-counter versions tend to wear out faster and often need frequent replacement.
Maintenance ensures comfort and hygiene.

Wearing a night guard may feel unusual at first. Expect mild tightness or increased saliva for a few days. Within one to two weeks, your mouth will adapt.
Most users notice reduced jaw stiffness or headaches after two to four weeks. For significant TMJ improvement, consistent nightly use over several months is key.
Schedule a follow-up with Buford Dentist to ensure your guard fits properly. Minor bite adjustments may be needed as your muscles relax. Regular checks prevent uneven wear or discomfort.
Contact your dentist if you experience:
These signs indicate the guard might need refitting or additional treatment.
Veneers are worth it if you want a fast, lasting way to improve your smile, provided you choose a qualified dentist and understand the costs, upkeep, and limitations. They deliver dramatic cosmetic results but involve permanent changes to your teeth and are not suited for every dental situation.
Veneers are thin shells bonded to the front of your teeth to improve appearance. They are custom-made to match the shape, size, and color you want.
Main types include:

Veneers deliver fast, noticeable results compared to other cosmetic dentistry options. At Buford Dentist, we see patients who want to fix:
Benefits include:

Veneers are a commitment. Once enamel is removed, it will not grow back. At Buford Dentist, we guide patients through these important considerations:
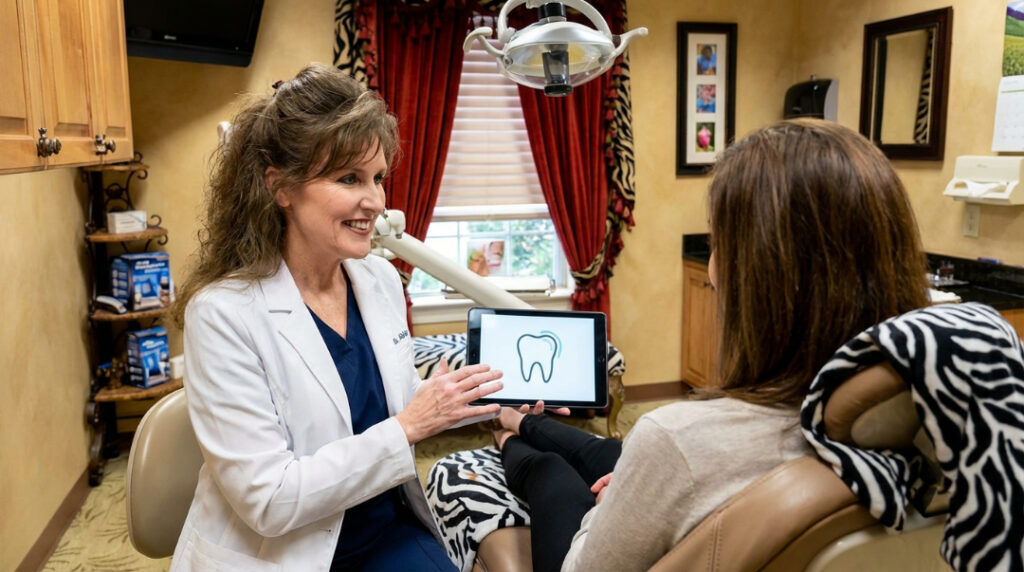
Getting veneers involves several steps:

Patients often ask about how long veneers last. Porcelain veneers typically last 10 to 15 years with proper care, while composite veneers last about 5 to 7 years. To maximize lifespan:

In Georgia, an alarming trend is the rise of unlicensed veneer providers promoting services online. Risks include:
Always verify your provider is a licensed dentist in Georgia. Ask for credentials and see before-and-after photos of real patients.

For some patients, other treatments are more practical:
A cost and benefit comparison often helps patients choose the right path.
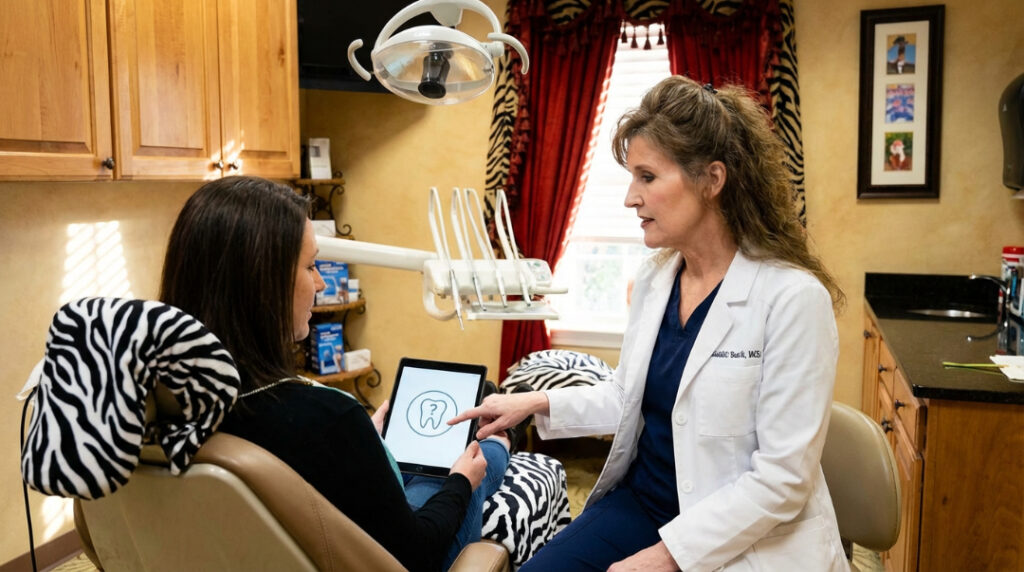
Before committing, ask yourself:
Booking a consultation with Buford Dentist will give you a tailored plan based on your goals, oral health, and budget.

Veneers offer dramatic improvement in your smile but require a permanent commitment. They are an investment in appearance and confidence, but success depends on:
When chosen for the right reasons and placed by a skilled dentist, veneers can be a lasting solution that transforms how you feel about your smile.
A regular dental cleaning, or prophylaxis, removes plaque and tartar above the gumline to maintain healthy teeth and gums. A deep cleaning, or scaling and root planing, removes plaque and tartar below the gumline and smooths tooth roots to treat gum disease. The main difference is prevention versus treatment.
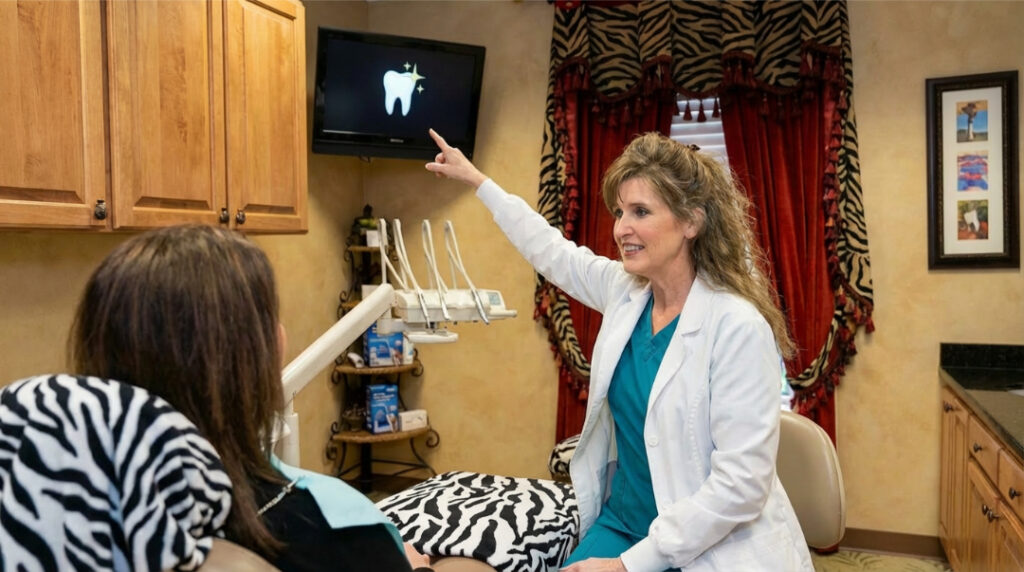
A regular dental cleaning is a preventive procedure for patients with healthy gums. It removes soft and hardened plaque above the gumline to prevent cavities and gum disease.
Typically, adults with healthy gums are advised to schedule a dental cleaning every six months. This timeline supports early detection of issues and consistent plaque control. However, the recommended dental cleaning frequency may vary based on individual risk factors such as smoking, diabetes, or a history of gum disease.
At Buford Dentist, we tailor cleaning intervals to each patient’s unique oral health needs. While many benefit from a standard twice-yearly schedule, some patients, especially those prone to cavities or gum issues may require more frequent visits to maintain optimal oral health.
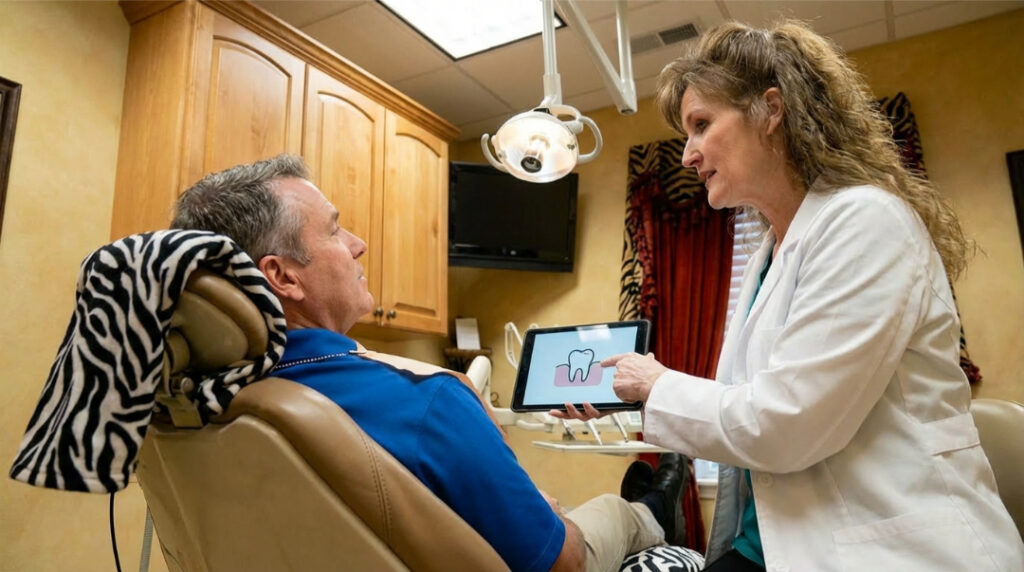
Deep cleaning is a therapeutic treatment for gum disease. It targets bacteria, plaque, and tartar below the gumline. The root surfaces are smoothed to help the gums heal and reattach.



Advances in dental diagnostics may make cleaning schedules more personalized. Saliva testing, genetic markers, and advanced imaging could help determine risk levels more accurately.
Most people should schedule a dental cleaning every six months to maintain healthy teeth and gums. Those with gum disease, high cavity risk, or other oral health concerns may need cleanings every three to four months, while individuals with excellent oral health could extend to once a year with a dentist’s approval.

Dental cleanings are essential for more than just a bright smile. They remove hardened plaque, called tartar, that regular brushing and flossing cannot eliminate. They also allow for early detection of gum disease, cavities, and other issues before they worsen. Poor oral health has been linked to systemic conditions like heart disease, diabetes, and respiratory infections.
Key benefits of professional cleanings:
The general recommendation is every six months. This guideline is supported by the American Dental Association as a baseline for healthy patients. Six months is enough time for plaque and tartar to build up to levels that require professional removal.
Why six months is the benchmark:
Not everyone needs the same cleaning frequency. Buford Dentist recommends customizing your schedule based on your oral health status, lifestyle habits, and medical history.
Low-risk patients:
Moderate-risk patients:
High-risk patients:
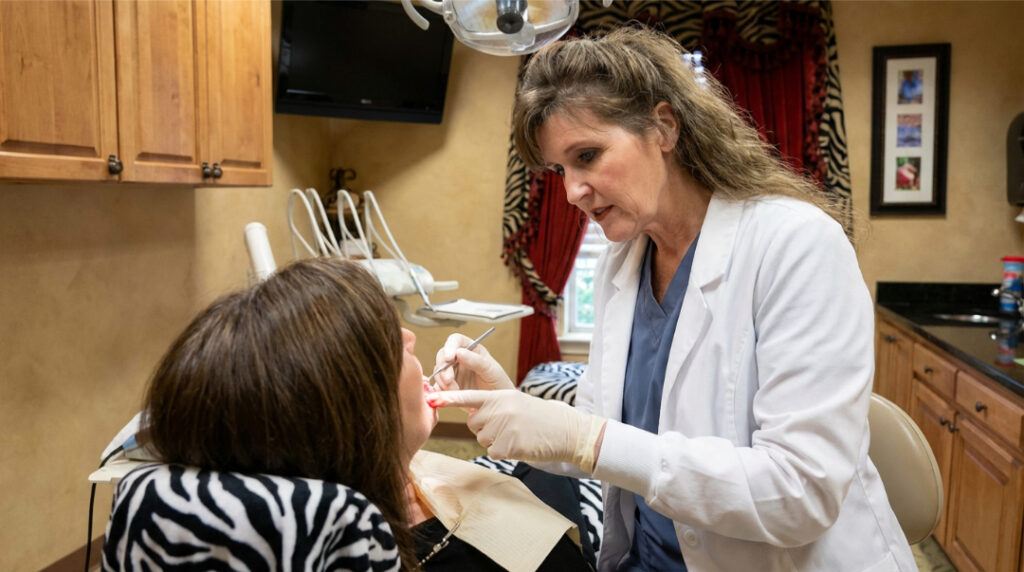
You may need to see your dentist earlier than planned if you notice:
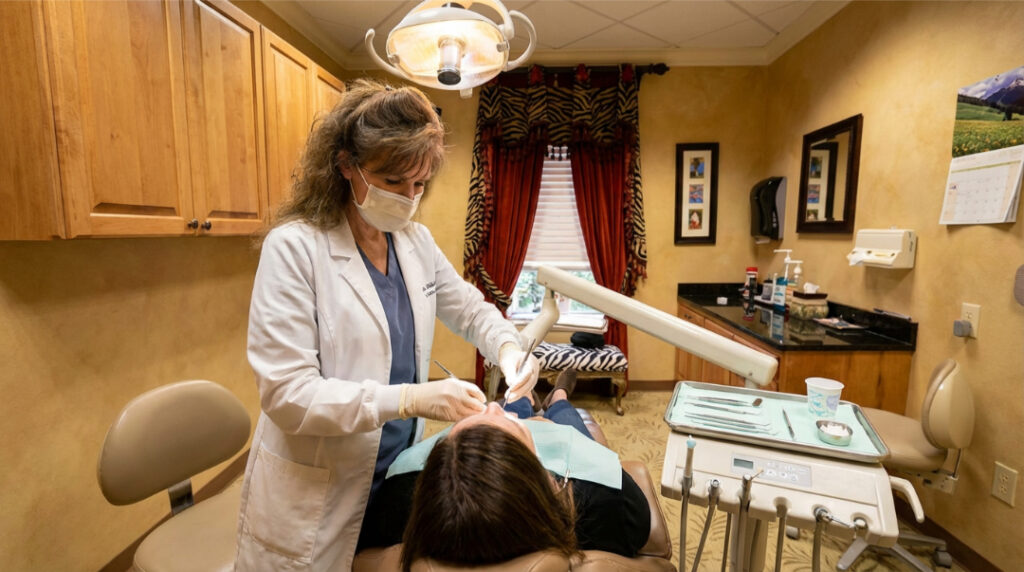
Professional cleanings at Buford Dentist are thorough and tailored to your needs.
Typical steps include:

Certain lifestyle and health factors increase the need for more frequent cleanings:

To find your ideal schedule, discuss these points with your dentist:

Professional cleanings are only part of oral health care. Daily habits keep your mouth healthy in between visits.
Recommendations from Buford Dentist:
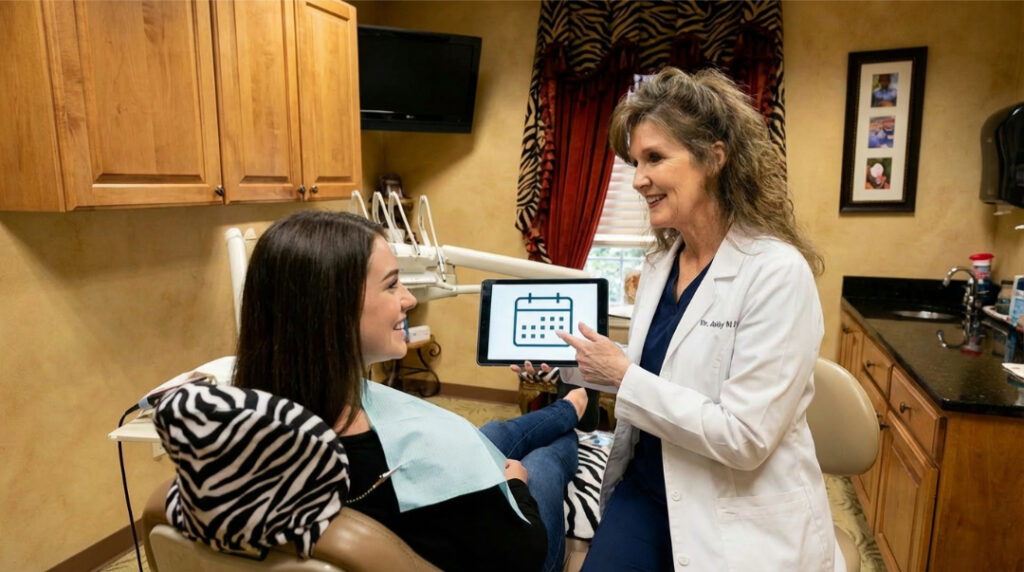
Different organizations and countries have varying guidelines when it comes to professional dental cleanings. However, it’s also important to understand the difference between dental cleanings, specifically, the contrast between regular preventive cleanings and more intensive deep cleanings. The type of cleaning you need can directly impact how often you should visit the dentist and what kind of care your gums and teeth require over time.
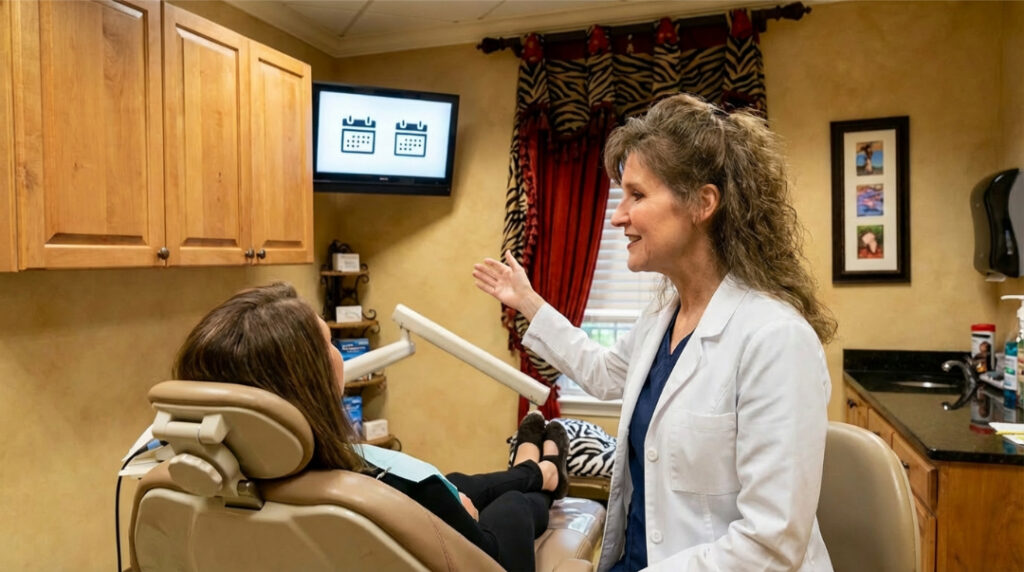
Studies have shown:
Advances in dental diagnostics may make cleaning schedules more personalized. Saliva testing, genetic markers, and advanced imaging could help determine risk levels more accurately.
No, as long as they are performed by a licensed professional.
No. Even with perfect brushing and flossing, tartar still forms and needs professional removal.
No. Deep cleaning treats gum disease and removes tartar from below the gumline.
Yes, children should typically have cleanings every six months unless otherwise advised.
You can usually start talking a few hours after wisdom teeth removal, but it's best to limit speaking as much as possible for the first 24–48 hours to allow proper healing. Excessive talking early on can increase your risk of complications like dry socket, bleeding, or delayed recovery.

Having your wisdom teeth removed is a common oral surgery, but the recovery phase often brings uncertainty—especially when it comes to talking afterward. At Buford Dentist, patients frequently ask, "How soon can I talk after wisdom teeth removal?" While everyone's experience varies slightly, there are general guidelines based on how your body heals and how complex your surgery was.
In this post, we’ll explore the timeline for talking, associated risks, practical communication tips, and signs to watch out for. By the end, you’ll know how to balance recovery with your daily communication needs—without compromising your healing process.

Why minimal talking is crucial:
Recommended strategy:
Tips for this phase:
At this stage:
However:

Everyone heals differently. Here are key variables that affect how soon you'll be able to talk:
Yes—but only when done mindfully.
Talking too early or too much increases the chances of:
Safe talking means:

Here’s how to navigate those early days when speaking is limited:
While these speech-related techniques are important, they work best when combined with broader tips for quick wisdom teeth recovery that support your body’s natural healing.

Phone calls can be deceptively stressful during recovery. Here's how to manage them:
You might be surprised at how many daily habits can affect your ability to speak comfortably:
Stay mindful. Rest is your best friend in the early recovery phase.

Excessive jaw movement is one of the biggest obstacles to recovery. Here’s what to know:
Stretching tip: After a few days, gentle side-to-side motions and slow opening exercises (as advised by your dentist) can restore flexibility.
Some discomfort while speaking is normal, but pain shouldn’t be sharp or increasing.
You may be experiencing:
If speaking is getting harder—not easier—each day, contact Buford Dentist immediately for follow-up care.

If you experience any of the following, don’t wait:
At Buford Dentist, we recommend a follow-up visit within a week to make sure you’re healing properly and can resume full function.
Yes, whispering involves less jaw movement. It’s safer than regular speech in the early hours post-op.
Text messages
Notepad or phone note apps
Gestures and expressions
Only after the third or fourth day, and keep it short. Video calls usually require more facial expression and engagement, which could strain your jaw.
Avoid singing for at least a week—it's too physically demanding on your jaw.
With early diagnosis, proper treatment, and consistent oral hygiene, many people with periodontal disease can keep their teeth for life. However, without treatment, periodontitis can lead to tooth loss in a matter of years, depending on severity and personal health factors.
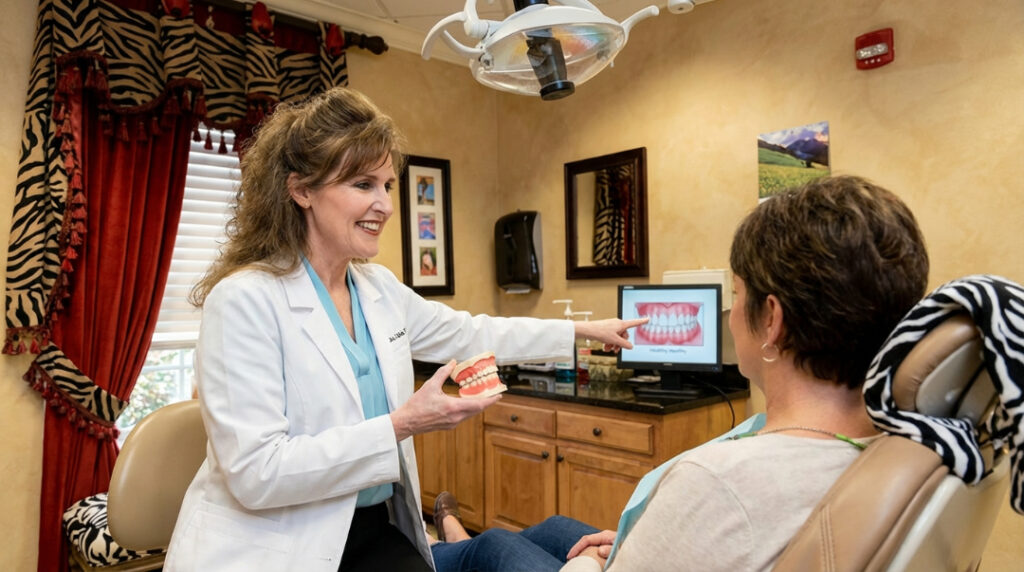
Periodontal disease, also known as gum disease, is one of the leading causes of adult tooth loss—but it doesn’t have to be. At Buford Dentist, we’ve seen firsthand how timely intervention and diligent care can help patients maintain their natural teeth for decades, even after a diagnosis of periodontitis.
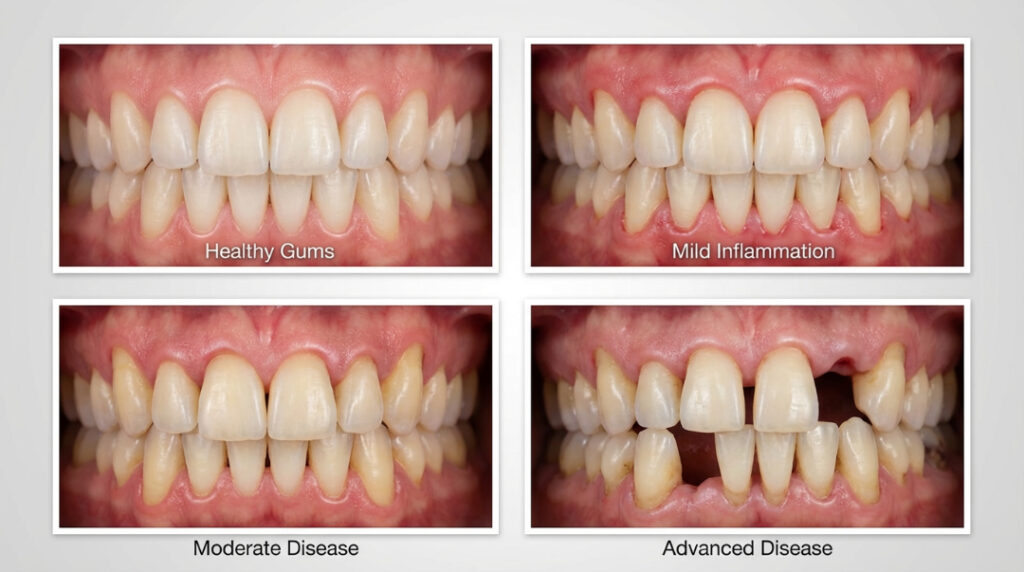
The timeline of tooth loss varies based on disease progression and patient response.
Without treatment:
With treatment:

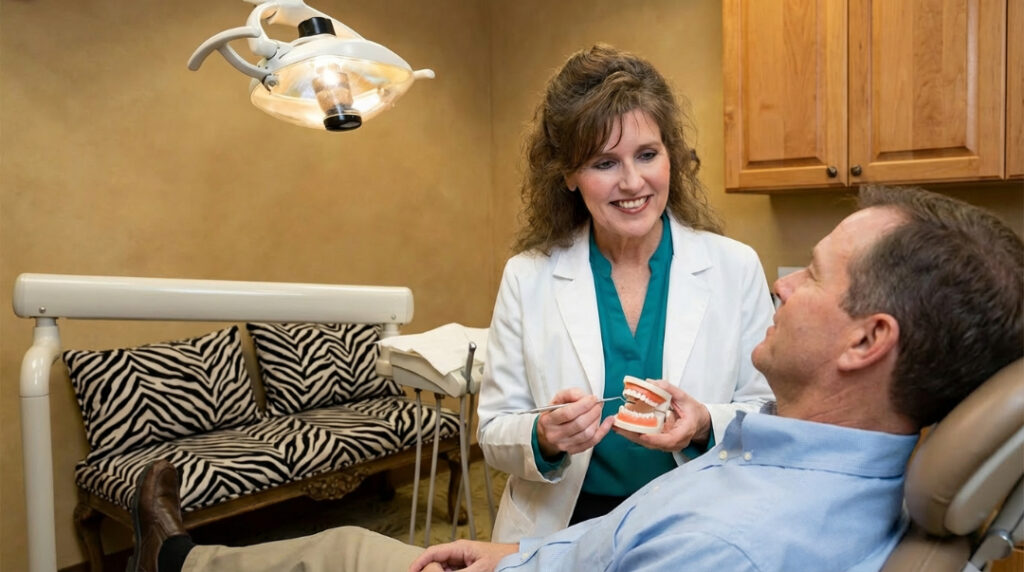
At Buford Dentist, we tailor treatments based on the stage of the disease and your overall health profile. These treatments include:
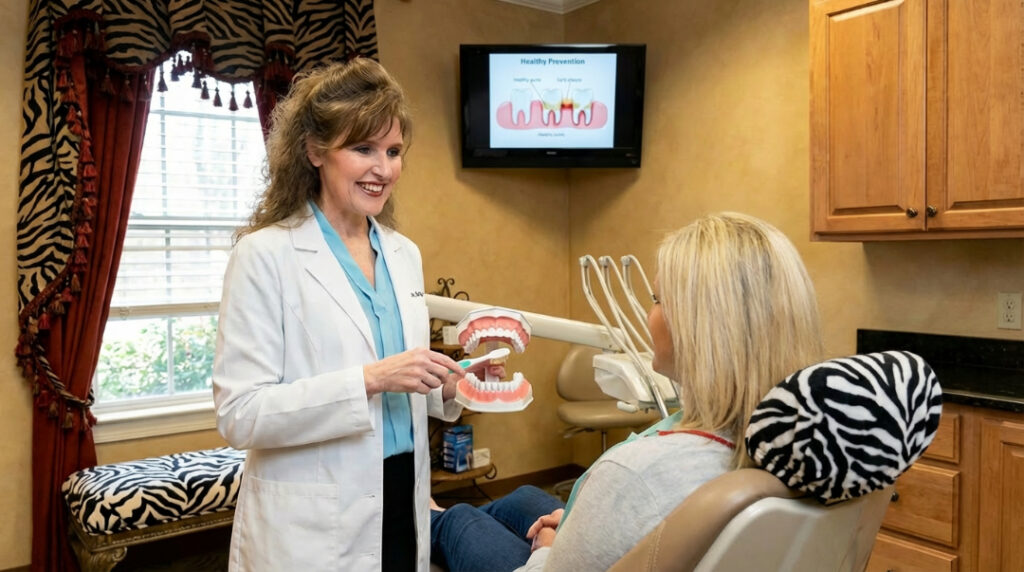
You can greatly reduce your risk of tooth loss by committing to these strategies:
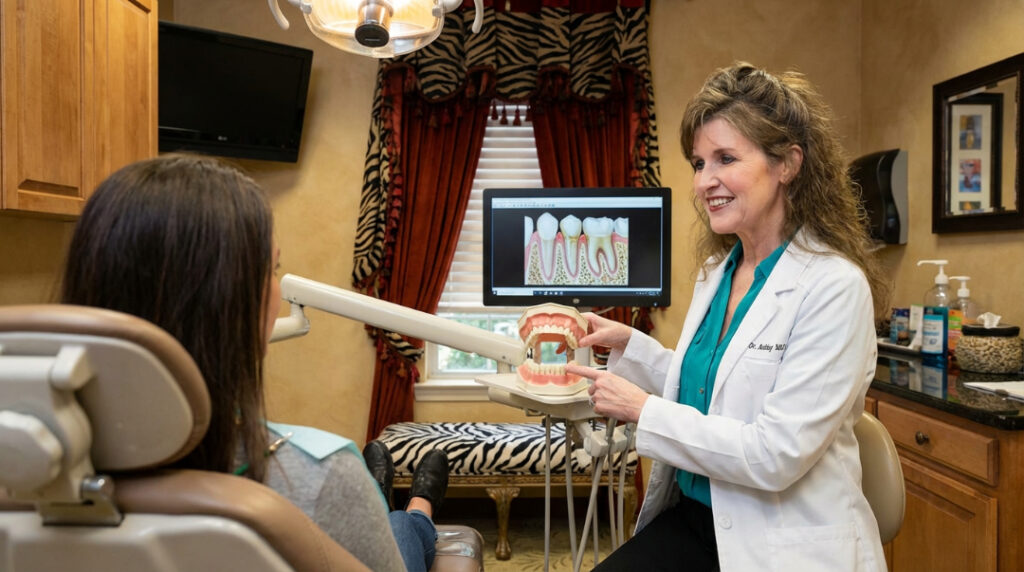
In some cases, despite all efforts, tooth loss may be inevitable. In these situations, modern dentistry offers highly effective solutions.
These options restore function, prevent neighboring teeth from shifting, and support facial structure.
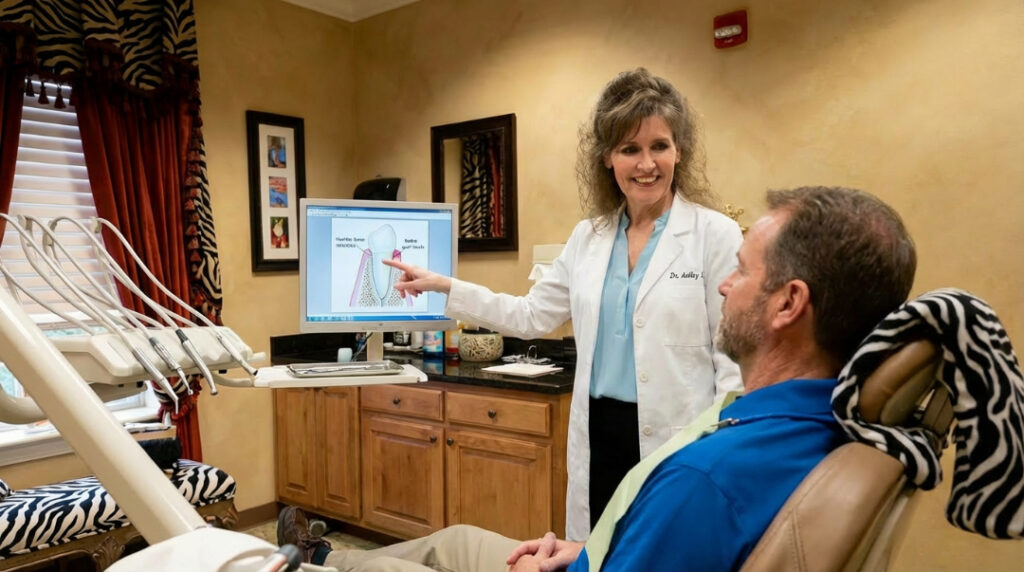
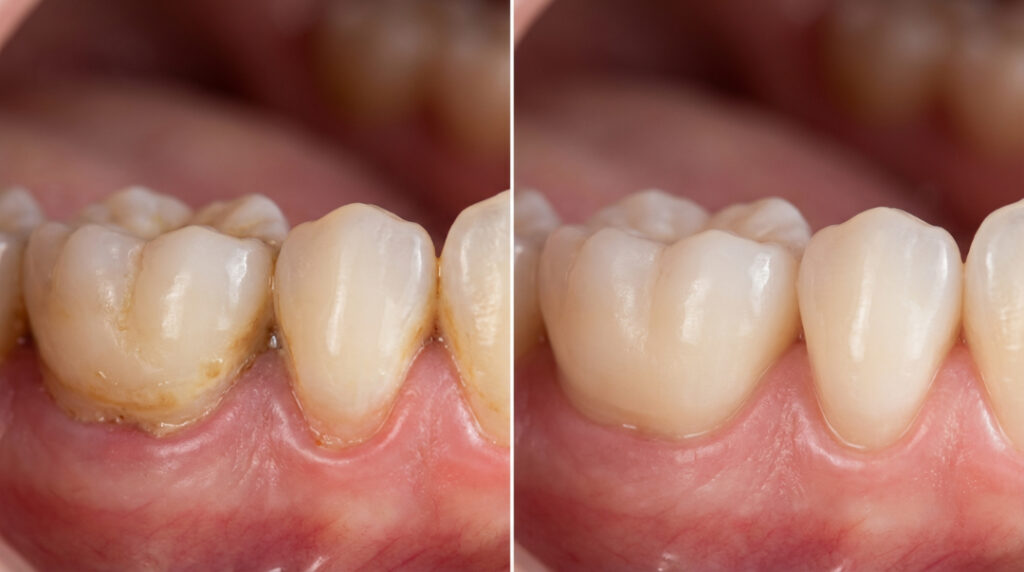
Let’s revisit this core non-surgical treatment. Scaling and root planing (SRP) is often underestimated, but it remains the gold standard for early to moderate periodontitis.
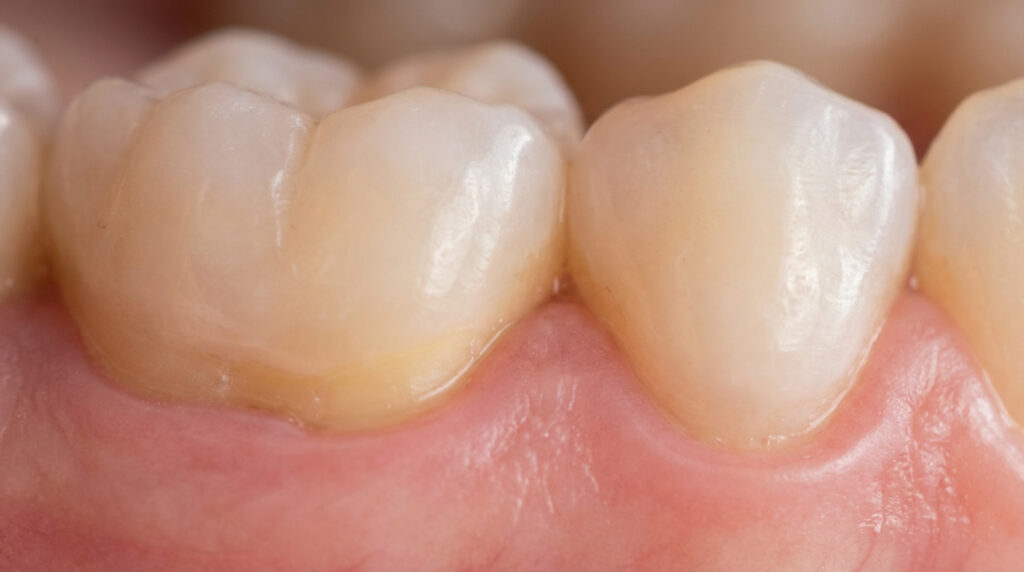
While the effects of periodontal disease can be managed, some damage may not be fully reversible.

Tooth mobility is a red flag that the supporting structures are failing. However, not all mobility means the tooth is lost.

We always tell our patients: once you've had periodontal disease, you’re at higher risk for recurrence. That’s why consistent Professional Dental Cleaning & Exams are critical for prevention and long-term health.
You can typically start eating spicy food 7 to 14 days after wisdom teeth removal, but only if you're no longer experiencing pain, swelling, or signs of slow healing. Always wait for your dentist’s green light and start with mild spices to avoid complications like dry socket or irritation.
Wisdom teeth removal is a common oral surgery, but returning to your favorite meals—especially spicy ones—requires caution. At Buford Dentist, we often get asked: “When can I eat spicy food again?” The answer isn’t one-size-fits-all.
Spicy food can:
That’s why a conservative approach to post-surgery meals is vital.
After extraction, your mouth goes through several healing phases. Knowing these helps you decide when it’s safe to eat spicy foods again.
Day 1–3: Blood Clot Formation
Day 4–7: Early Healing Begins
Week 2–3: Continued Healing
Week 4 and beyond: Bone and Tissue Maturity
Eating spicy foods too soon can cause:
Capsaicin, the compound in spicy food, acts like sandpaper on a wound—it doesn’t just burn; it disrupts the healing tissue.
There’s no perfect calendar date, but general guidelines are:
Minimum of 7 days for straightforward extractions
Up to 14 days for more complex or surgical removals
Longer for smokers, diabetics, or those with poor healing
These timelines can vary, so always consider your individual recovery progress. If you're unsure about how your healing is going, consult your provider — especially if you're still early in your recovery from a tooth extraction.
Before trying spicy food again, ask yourself:
If you answered yes to all three, you may cautiously test with mild spice.
Look for these recovery milestones before spicing up your meals:
If you still feel pressure or sensitivity in the area, wait a few more days.
When you finally indulge in spicy food again, ease back in. Here’s how:
If you feel a burn or sharp pain, stop and wait a few more days.
Even after your stitches are gone, some foods can cause setbacks. Avoid:
Craving flavor without the heat? Consider:
These keep your meals tasty while staying gentle on your gums.
If you’ve tried spicy food and noticed discomfort, don’t panic—but don’t push through either.
Stop and:
Early action helps prevent complications.
While general advice is helpful, your healing is personal. Consult your dentist if:
At Buford Dentist, we provide personalized aftercare plans to guide your diet, hygiene, and recovery. Never hesitate to ask questions—it’s better to delay spicy food than to delay healing.
Here’s a simplified guide to eating after wisdom teeth removal:
First 24 hours
Days 2–3
Days 4–7
Week 2 and beyond